New Hire Enrollment for
Out-of-State Workforce
Wherever you’re from, you’re welcome at ECU Health.
Please take a moment to enjoy this video, especially for our newest team members.
Welcome! We understand that your life is so much more than just your time at work. That’s why our total rewards package is diverse, comprehensive, and full of benefits built to support you.
You’ll find all the information you need right here on this site. Be sure to bookmark it and share it with your family too. (And be sure to call in during Benefits Office Hours if you or your family has questions. See below.)
Care Anytime, Anywhere Through ECU HealthNow
You can use ECU HealthNow to connect with a provider 24/7 by phone or online. If you are enrolled in the Medical Savings Plan, there is a $55 fee for service until your deductible has been met.
Visit ECU HealthNow or download the ECU HealthNow app from your app store.

Check the Date!
As a new team member, you must enroll in benefits online within 30 calendar days of your date of hire, or the date you become benefits eligible.
Network Guide
If you and/or your eligible dependents reside outside of North Carolina, you will have access to medical provider networks specific for our out-of-state workforce. You will have access to the following networks based on the location of your residence:
- National: First Health
- North Carolina/South Carolina/Virginia: MedCost/Viginia Plus
- New York/New Jersey: Magnacare
- West Virginia: 4Most
Your network will be listed on the medical cards mailed to your home address. The address on record for team members and any out-of-state dependents will determine the card that is mailed. Team members with dependents residing in another state should notify HR Services of the dependent’s address. MedCost will issue a specific ID card for that dependent with the primary network for their state.

Key Terms to Know
First Health is an NCQA-accredited Provider Network that has strong provider relationships with more than 5,700 hospitals over 120,000 ancillary facilities, and over 780,000 professional providers at over 1.5 million health care service locations across all 50 states.
How do team members find a provider within the First Health Network?
- Go to medcost.com (link to Directory)
- Click on “Find a Doctor or Facility”
- Click on the drop-down and choose the network called “ECU Health Plan Provider Directory“
- Click on “Virginia Residents and Outside of NC, SC & VA”
- Click on “First Health Network (Travel Network)”
Please note First Health, Magnacare and 4Most do not have accessibility to:
- The ECU Health Employee Pharmacy due to geographical location.
- ECU Health Alliance (Tier 1) pricing due to geographical location (this may also be true for some plan members in the MedCost/Virginia Plus network).
New Team Member Checklist
Explore the benefit options available to you by reviewing your Benefits Guide and premiums.
Review your medical expenses over the past year and estimate how much you will need to contribute to a Flexible Spending Account (FSA) or Health Savings Account (HSA). You must be enrolled in the Medical Savings Plan to participate in the HSA.
Gather this information before you enroll:
- For you: Your ECU Health UserID and password.
- For your dependents and beneficiaries: Social Security numbers, addresses and dates of birth.
Verify (or update) your mailing address.
To enroll, click the “Enroll” button in the upper right-hand corner, enter your team member ID and password and elect or waive each benefit.
If you do not wish to cover yourself and eligible dependents using our benefit offerings, log into Employee Self Service, designate beneficiaries where applicable and decline the remaining benefits. Remember, you must take action to make sure you have the coverage that is right for you and your family. If you do not enroll, you will only have employer-paid benefits.
After you enroll your spouse and/or eligible dependent child(ren), you will receive a packet from the dependent verification center. You will need to provide documentation to ECU Health’s dependent verification center to confirm your dependent’s eligibility for coverage.
Acceptable Forms of Documentation include:
- Marriage license for spouse.
- Domestic partner attestation.
- Birth certificate for children.
- First page of your most recent tax return, listing eligible dependents (for spouse and/or children).
- Court-ordered guardianship papers, adoption papers or placement letter.
- Divorce decree to show parent/child relationship when names don’t match or to identify responsibility for providing health coverage.
You and ECU Health share the cost of your benefits. Your share will automatically be deducted from your ECU Health paycheck on a before-tax basis.
All new hires and first-time eligible team members are automatically enrolled in the 401(k) plan at 5% of your earnings after 30 days from your start date, or as soon as administratively practical.
2024 Benefits Guides
Find all of the details you need to know about your plan in your benefits guide.
2024 Premiums
Are you part-time or full-time? You’ll find details about the premiums here.
Full-Time Team Members—Bi-Weekly Deductions
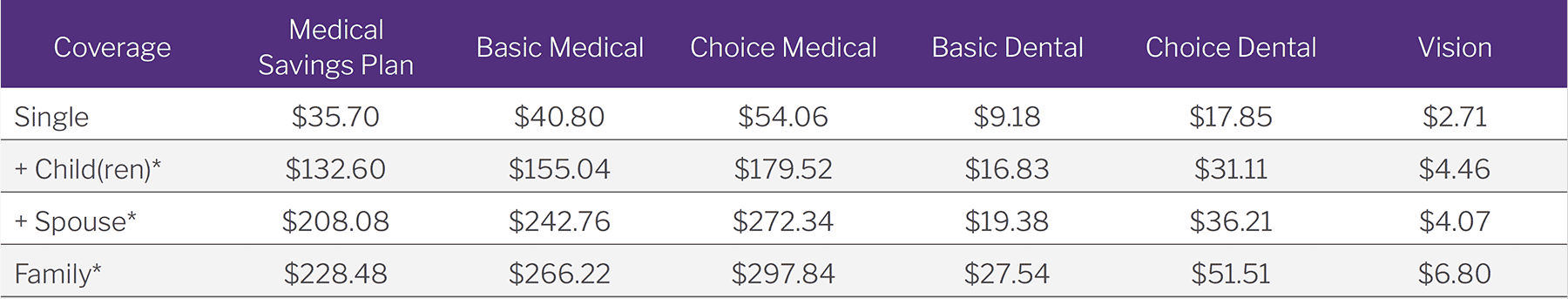
* Includes domestic partner/domestic partner’s children.
Part-Time Team Members—Bi-Weekly Deductions
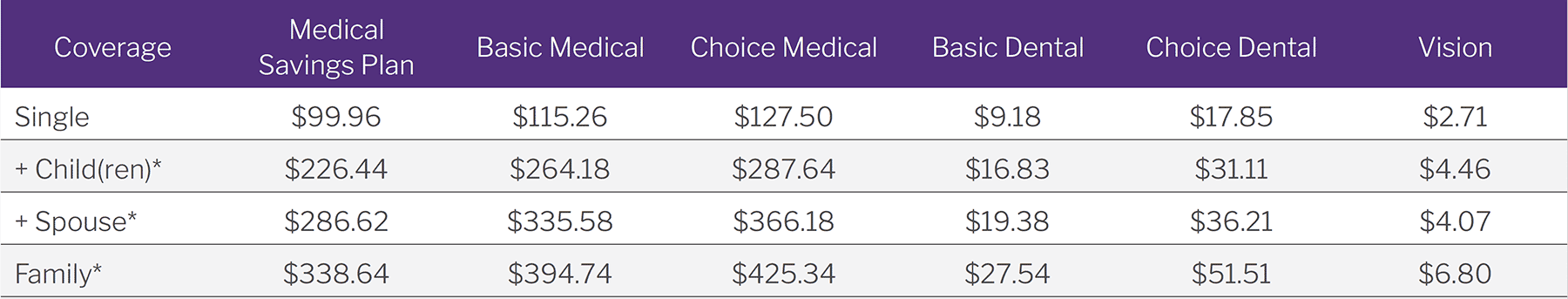
* Includes domestic partner/domestic partner’s children.
Have questions? Get them answered.
Questions? AskPhin!
Visit AskPhin.com or call 252‑816‑PHIN (7446).
Like videos?
Check out the Virtual Benefits Fair for more info.
Join us on Mondays from 3 – 4 p.m. EST for Benefits Office Hours to get answers to any benefits-related question.
Scan the QR code to join by video OR visit: bit.ly/BenefitsOfficeHours
Join by phone: 650-479-3208 Call-in toll number (US/Canada)
Meeting number: 2314 863 3828 (access code)
Meeting password: Benefits